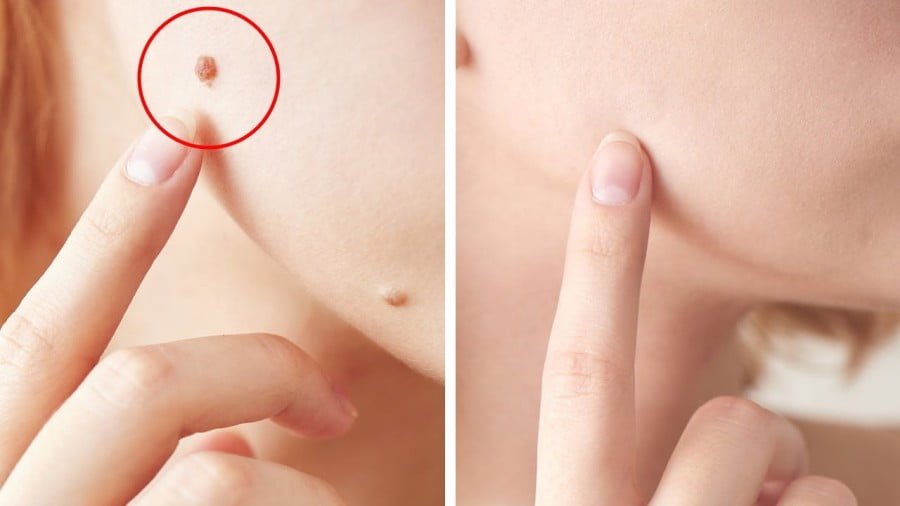
Do Your Moles Ever Go Away?
Skin is your body’s largest and fastest growing organ, used to protect your body from bacteria and germs, regulate your temperature, get rid of waste products and house a nervous system that allows you to feel and sense your environment.1 Your skin is what others first notice about you, and is an indicator of both internal and external aging.
Skin cancer is one of the most common types of cancer in the U.S.2 Estimates suggest nearly 20 percent of all Americans will experience some form of skin cancer during their life. Non-melanoma skin cancers affect nearly 3 million Americans each year and more than 1 million are living with melanoma. The rates of diagnosis of basal cell (BCC) and squamous cell carcinomas (SCC), non-melanoma skin cancers, have been rising dramatically.
There has been an increase of 145 percent of BCC between 1976 to 1984 and 2000 to 2010, and a 263 percent increase of SCC during the same period.3 Routinely inspecting your skin increases the likelihood you’ll recognize changes that may need medical attention, and will help you become more familiar with your unique pattern of moles (nevi), freckles and blemishes.
Monthly self-inspection is done in a well-lit room with the assistance of mirrors to inspect areas that are difficult to see. Your first examination may take longer as you record the location of moles and freckles on your body. This enables you to confirm the location and any changes each month forward. You might notice that a mole suddenly appears where there wasn’t one before, or a mole you’ve had for years may start to disappear.
Evolution of a Mole
Moles are growths on your skin that are usually black or brown, but can be a lighter tan. They usually appear in childhood anywhere on your body, either alone or in groups. By the time you reach your mid-20s it’s common to have 10 to 40 moles.4 Moles happen when cells that provide color to your skin — melanocytes — grow in clumps together instead of spreading throughout your skin. After being exposed to the sun or during hormonal changes, such as your teen years or pregnancy, moles may darken in color.
Not all moles are created equally. The common mole is 5 to 6 mm in diameter, with distinct edges and evenly pigmented.5 Congenital nevi are present at birth, can range in size and shape and are sometimes referred to as birthmarks, while acquired moles appear during childhood or young adulthood. Congenital nevi have a higher risk of developing into melanoma as you age.6
When the shape and size of your mole is uncommon, it’s called dysplastic nevi.7 Sometimes called “atypical moles,” these dysplastic nevi may be larger than a common mole, range in color from pink to black and have both raised and flat areas on the mole. The area may be slightly scaly, and the edges may not be defined and can occur anywhere on the body. If you have dysplastic nevi, you also likely have a larger number of common moles.8
Moles are classified according to the layers of skin in which they appear, between the dermis and epidermis (junctional), in the dermis (intradermal) or in both the dermis and the junction between the dermis and epidermal layers (compound).9 Halo nevi are raised moles that develop a ring of lighter pigmented skin around the mole, likely from inflammatory infiltrating cells. Why the reaction occurs is not known, but halo moles are benign and don’t require treatment.
Disappearing Nevi
While not common, some moles may disappear. Some of the more common reasons they fade are hormonal changes associated with pregnancy or the evolution of change over time.10 During pregnancy, it is not unusual for moles to darken in appearance. After birth, these moles will lighten, sometimes so much so they appear to have disappeared.
Sometimes a healthy mole will disappear over time, but the process is usually gradual. The mole usually starts out flat, becomes slightly raised and then becomes lighter and pale, eventually disappearing.11 These disappearing moles are not usually cause for concern unless your physician has previously flagged the mole as possibly problematic.12
Although any mole can appear or disappear, halo moles are known to go through a yearslong process as they fade from view.13 The process starts when pigmentation is lost around the mole and a pale white ring forms. Over time the mole itself fades, leaving skin lighter than the surrounding pigmentation. In the coming years melanocytes will spread over the area and it blends in with the surrounding skin.
Is Your Mole Cancerous?
Although it isn’t unusual for a mole to appear or disappear, there are instances when a mole has become cancerous and then disappears, while the cancer has spread to other areas of your body.14 A disappearing mole is not often a sign of cancer, but it is worth investigating, especially if the mole had an unusual appearance, changed before fading, faded rapidly or had been dysplastic.15
When an area of skin becomes cancerous, your immune system will fight back, sometimes reducing the size of the cancerous mole or making it disappear altogether. It the cancer has not metastasized, then the disappearance or regression of the mole is a cure.16However, if the cancer has spread, the disappearance of the initial site does not mean the cancer has resolved. As you inspect your body for changes in your moles, look for the following signs that may mean a mole is transitioning to a melanoma skin cancer. The ABCDE rule makes it easier to remember the signs:17
A: Asymmetry is when one half of a mole doesn’t match the other half
B: Borders are not well-defined, but rather ragged, irregular, notched or blurred
C: Color of the mole is not the same throughout the mole
D: Diameter is larger than 6 mm or the width of a pencil eraser
E: Evolving over time, the mole is changing in shape, diameter and color
Non-melanoma BCC or SCC may have different symptoms.18 In these cases, an unusual growth or sore that doesn’t resolve quickly may be the first indication. Initially, you may see a nodule, rash or an irregular patch that may be raised and likely oozes or bleeds easily. You may see blood vessels or an indentation in the center of a developing BCC, while SCC may progress as firm lumps with a rough surface that develops slowly.
Deadly Melanoma Related to Your Degree of Sun Exposure
A 10-year multicenter survey published in the Journal of the American Academy of Dermatology found early removal of suspect skin lesions, with the intent to reduce mortality from melanoma, may not be effective as many of the lesions removed were benign and the procedures led to further morbidity and health care costs for the patients.19 Further, the researchers found it was the specialized clinics that became more adept at differentiating benign from cancerous moles.
This should not be surprising, as professionals who analyze more skin lesions will become more adept at identifying those that require treatment. Thus, if you find a suspect mole or lesion it is important to seek an evaluation by a specialized clinic until you are satisfied with the analysis. However, while your risk of developing a deadly melanoma is related to sun exposure, it is too little exposure that raises your risk and not too much.
While the death rate from melanoma has remained stable, new cases have risen by 1.4 percent each year over 10 years.20 Rising rates have been largely blamed on sun exposure, and dermatologists warn you should wear heavy sunscreen protection anytime you are in the sun. However, while many sunscreen products protect your skin against UVB light, they are relatively ineffective against UVA unless you use one that can effectively screen out both.21
UVB light is the spectrum of ultraviolet light responsible for sunburns and blistered skin, while UVA light penetrates more deeply, triggering cellular damage leading to cancerous growths. The amount of UVB light fluctuates through the year as there is less intensity when the sun rides lower in the sky during the winter months, but no such fluctuation occurs for UVA light.22 UVB light is also what your body uses to produce vitamin D.23 Taken together, this means slathering on sunscreen products may be reducing your vitamin D production without actually protecting your skin from the most damaging UVA radiation.
Are You Increasing Your Risk of Death by Avoiding the Sun?
A study published in the Journal of Internal Medicine found avoiding sun exposure increases your risk from all-cause mortality.24 The researchers followed nearly 30,000 middle-aged to older women over a span of 20 years in Sweden. The data indicated that chronic sun exposure was associated with a reduced risk of mortality, which is in direct conflict with nearly every dermatologist’s recommendations.
Another study found the rates of melanoma are increasing at a greater rate among fair-skinned indoor workers since 1940, possibly since UVA rays easily penetrate large windows while UVB rays do not, thus negatively affecting production of vitamin D and increasing cellular damage from UVA.25 Many studies have shown having sufficient vitamin D helps protect against many forms of cancer26 and improves the health of your bones and teeth,27 immune system,28 cardiovascular system29 and brain.30
If dermatologists’ recommendations were correct, then the incidence of skin cancers should be decreasing as use of sunscreen products have become more popular. However, over the past 30 years these rates have only increased. Many sunscreen products also contain toxic ingredients and vitamin A that has been shown to increase the speed of malignant cell development and the spread of skin cancer.31
Simple Skin Cancer Prevention Strategies
As with most medical conditions, prevention is the best medicine. Your skin was designed to produce vitamin D, and when done properly is the best way to reduce your risk of many different diseases, including skin cancer. In combination with optimizing your vitamin D levels, the carotenoid astaxanthin has a unique ability to reduce signs of aging by protecting your skin from sun damage.
Eating a healthy, whole food diet, rich in natural antioxidants is another useful strategy to avoid damage to your skin. While you want to shield yourself from burning, you also want to get healthy, sensible sun exposure to optimize your vitamin D. Sunlight also has many other health benefits over and above vitamin D production. Here are a few tips to help you reap the maximum reward while minimizing your risk:
- Expose large amounts of your skin to sunlight for short periods daily. By exposing at least 40 percent of your body, you increase your chances of producing adequate amounts of vitamin D. If you are going to use sunscreen, give your body the chance to produce vitamin D before you apply the product, and choose a product that is nontoxic and protects against both UVA and UVB light. The Environmental Working Group publishes a comprehensive “Guide to Sunscreens.”32
- Use a large hat to shield your face from the sun, as the skin on your face is thinner and more prone to damage.
- Stay out long enough for your body to turn the very lightest shade of pink if you’re light-skinned, or just a hint of reddish if you’re dark-skinned. Cover with clothing, hat or shade if you are planning to stay out for a longer period. If natural shade is not available, create your own shade using an umbrella.
- Astaxanthin is a powerful way of protecting your skin internally from exposure to UVA rays. It typically takes several weeks of daily supplementation to provide protection by saturating your body’s tissues.
Sources and References
- 1 American Academy of Dermatology, About Skin
- 2, 3 American Academy of Dermatology, Skin Cancer
- 4, 6 WebMD, Moles, Freckles and Skin Tags
- 5, 9 Skin Vision, April 5, 2016
- 7, 8 National Cancer Institute, Common Moles, Dysplastic Nevi and Risk of Melanoma
- 10, 11, 14, 15, 16 Medical News Today January 23, 2018
- 12, 13 Healthline, June 20, 2017
- 17 American Cancer Society, Signs and Symptoms of Melanoma Skin Cancer
- 18 Cancer Treatment Centers of America, Skin Cancer Symptoms
- 19 Journal of the American Academy of Dermatology, 2012;67(1):54
- 20 National Cancer Institute SEER, Melanoma of the Skin
- 21, 22 Environmental Working Group, September 28, 2010
- 23 Journal of Pharmacology and Pharmacotherapeutics, 2012; 3(2):118
- 24 Journal of Internal Medicine, 2014;276(1):77
- 25 Medical Hypothesis, 2009; 72(4):434
- 26 National Cancer Institute, Vitamin D and Cancer Prevention
- 27 WebMD, Keep That Smile!
- 28 Journal of Investigative Medicine, 2011;59(6):881
- 29 Johns Hopkins Medicine, Vitamin D and the Heart
- 30 Scientific American, November 1, 2009
- 31 Environmental Working Group, The Problem with Vitamin A
- 32 Environmental Working Group, Guide to Sunscreens
By Dr. Joseph Mercola
Source: Mercola